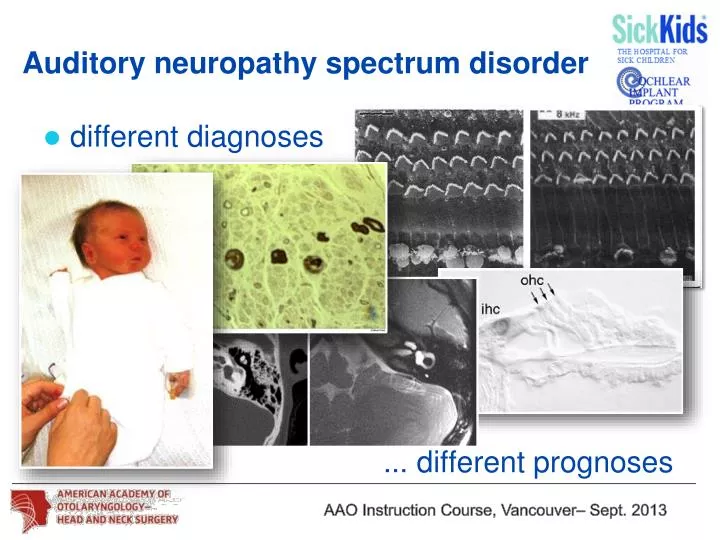 
Also, in many cases, sometimes because of co-occurring disabilities, patients cannot respond appropriately during behavioral audiometry. In addition, there are populations of hearing-impaired patients who cannot tolerate general anesthesia because of concomitant disabilities. The use of general anesthesia for a threshold ABR and ASSR, while usually effective, has the potential to be dangerous and stressful for children and parents and is more expensive than nonsedated ABR (e.g., Cotè et al., 2006 Francois et al., 2012 Reich & Wiatrak, 1996). Though advancements in recording equipment and data processing techniques may help with some patient-related artifact, when a pediatric patient will not submit to ABR or ASSR testing on his or her own accord, sedated testing is frequently recommended. Thus, as infants become young children, sleep less, and are typically more active during waking hours, ABR and ASSR techniques often prove inadequate. Furthermore, both the ABR and ASSR require patients to be asleep or extremely still in order to record useful evoked potential data. In this population, the ABR and ASSR are typically absent or grossly abnormal due to decreased synchrony of the auditory nerve and brainstem and, therefore, cannot provide any information regarding hearing threshold (e.g., Rance et al., 2005 Starr et al., 1996). One major example of such confines is found in children with ANSD. While this practice has proven effective in the majority of patients, it has several limitations. Currently, the ABR and the ASSR are ubiquitously used to identify and diagnose hearing loss in newborns and young children. The use of physiologic means of estimating auditory threshold has made great contributions to early identification and treatment of hearing loss. 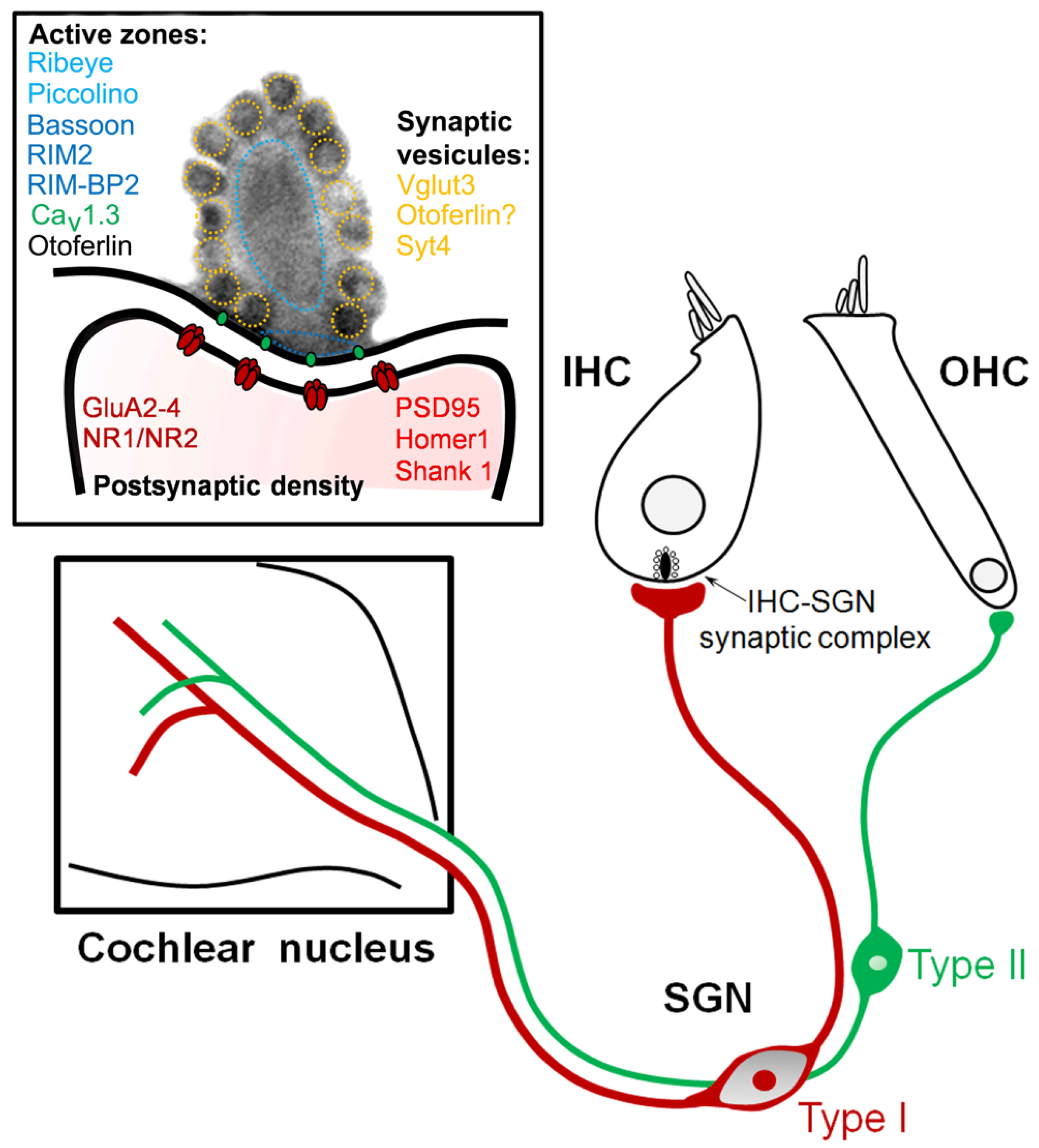
Defined as the lowest intensity at which a person can correctly identify the presence of a sound 50% of the time ( Katz, 2002), auditory thresholds are used in characterizing the severity of hearing loss, providing prognoses for patients with hearing loss, and in treatment (e.g., in hearing aid fitting). 
The obtaining and use of auditory thresholds is pervasive in the field of audiology. The clinical utility of CAEPs as a tool to estimate auditory threshold is further demonstrated with one case of pediatric sensorineural hearing loss (SNHL) and two case studies of children with auditory neuropathy spectrum disorder (ANSD). Here, we also expand on previous work by presenting a novel adjustment to traditional CAEP threshold estimation methods, which serves to shorten test time while still preserving reasonable accuracy. Thus, the current study aimed to investigate and replicate the effectiveness and feasibility of CAEP threshold estimation in both children and adults with normal hearing (NH). However, as we will describe, there are many individuals who could benefit from the use of CAEPs to measure auditory threshold, in lieu of or in addition to currently standard clinical methods. To a large degree, threshold estimation using CAEPs has not been widely accepted as a clinical technique, due to the wide usage of other evoked potentials, such as the auditory brainstem response (ABR) and auditory steady state response (ASSR), for clinical threshold estimation (see Sininger et al., 2018, for a review) and other limiting factors of CAEP testing, including test session duration. A relatively extensive literature that dates back several decades provides evidence supporting this notion (see Cone-Wesson & Wunderlich, 2003, for a review). Cortical auditory evoked potentials (CAEP) can be used as a physiologic means of estimating auditory threshold.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
